practice research | 2026
Caring about Care
What is missed in the community of care?
A report of a discovery journey into dementia caregivers' life and experience.
Introduction
Caregiving can be a painful, loving, and deeply draining experience at the same time. This was my initial understanding as someone who had witnessed a family member caring for an ageing person living with dementia for almost a decade. As a designer, I kept returning to one question: how might design offer support within such a complex and emotionally difficult situation?
When I began this research in September 2025, my intention was to design something that could make life easier for older people living with dementia, and therefore make life easier for their caregivers too. At that stage, I imagined the outcome might be a product, a service, or a practical tool. However, after the first phase of my research, this intention shifted significantly. I began to realise that one of the most overlooked pillars within the community of care is not only the person receiving care, but the unpaid caregiver.
This phase of research therefore focuses on understanding the community of care from the perspective of unpaid caregivers. I wanted to explore their lived experience: what they carry, what they lose, what support they receive, and what remains missing. Through this, the project began to ask a different question: how can design approach the needs of unpaid caregivers, not as secondary figures in the care system, but as central participants whose wellbeing directly shapes the quality and sustainability of care itself?
Literature Review
Existing literature on caregiving shows that family caregivers often occupy a difficult and contradictory position: they are central to care, yet their labour is frequently unsupported and under-recognised. Kate Washington's Already Toast frames unpaid caregiving as an all-consuming role shaped by burnout, lack of support, and structural failure. This closely connects to what emerged in my interviews, where caregivers repeatedly described the emotional and practical weight of care, as well as the absence of sufficient support around them.
The Care Manifesto by The Care Collective also positions care as a social and political issue, rather than only a private family responsibility. This perspective is important to my research because it suggests that caregiving should not be understood only as something that happens inside families, but as something shaped by wider systems, values, and social structures.
Within dementia-specific care, Anne Basting's Creative Care offers a more relational and creative approach, shifting attention away from purely clinical models and towards connection, imagination, and lived experience. This has helped me think about how creative practice might engage with dementia care beyond problem-solving alone.
Qualitative studies of dementia caregiving also identify recurring experiences such as exhaustion, sadness, frustration, social isolation, and the difficulty of understanding dementia as it changes family relationships. These sources help position my own research with 16 participants, where similar patterns appeared repeatedly: being thrown into the situation without knowing what to expect, emotional weight, isolation, repetition, and the feeling of being overlooked within the wider care system.
Research Approach
My research included interviews with 10 unpaid caregivers and 6 witnesses, all of whom were family members of caregivers. The participants came from Iran (5), the UK (4), India (3), Jamaica (1), Canada (1), Korea (1), and Sweden (1).
All of the caregivers I interviewed were caring, or had cared, for a parent rather than a partner. This is important to acknowledge, as it adds a specific emotional and relational layer to the research. Caring for a parent may involve different responsibilities, expectations, and forms of grief than caring for a partner. This is a layer I have not explored fully at this stage, but it is important to recognise.
Alongside the interviews, I also used the Alzheimer's Society platform to collect and review 45 stories shared by users about their experiences of dementia caregiving.
The interviews were conducted in a free-flowing style. I had a list of questions, but because the topic was sensitive, I preferred to let each conversation move in the direction the interviewee felt comfortable with. I usually began by asking them to tell me their story. Although I expected these conversations to be difficult, apart from one case, all of the interviewees were very open and willing to share their experiences.
In most of the interviews, I collected much more information than I had expected when I first structured the questions. The longest interview lasted almost two hours. All interviewees gave consent for the information they shared to be used anonymously.
Each interview unfolded differently, but I tried to cover the following questions in all of them:
- What was the main reason for care? For example, dementia, stroke, ageing, or another condition.
- How long had the caregiving situation lasted?
- What were their feelings during this experience?
- What felt missing?
- What would they change if they could?
- What would they say to someone who had just become a caregiver?
- What technology, support, or resource helped them the most?
These were also the same points I looked for while reviewing the online stories shared on the Alzheimer's Society platform.
My questions were structured around the caregiving situation itself, in order to understand the community of care more clearly. However, the interviews gradually shifted my approach from focusing mainly on the person receiving care to focusing on the caregiver.
To summarise the experience in one word, I would say that caregivers experience invisibility in their lives. They are pressed between different responsibilities and expectations, while also carrying the emotional, and in many cases economic, pressure of the situation. There is often very little time, energy, or space left for themselves.
This is especially important because the caregiver's wellbeing directly affects the quality of care they are able to give, and therefore also affects the wellbeing of the person living with dementia. After this point in my research, I redirected my project towards unpaid caregivers as one of the most overlooked pillars within the community of care.
The Conversations
What I heard / What kept repeating
Figure 2 presents a system map extracted from interviews and case studies. As the map shows, different feelings, difficulties, challenges, and structural gaps are deeply interlinked. It is very difficult to consider any one aspect in isolation.
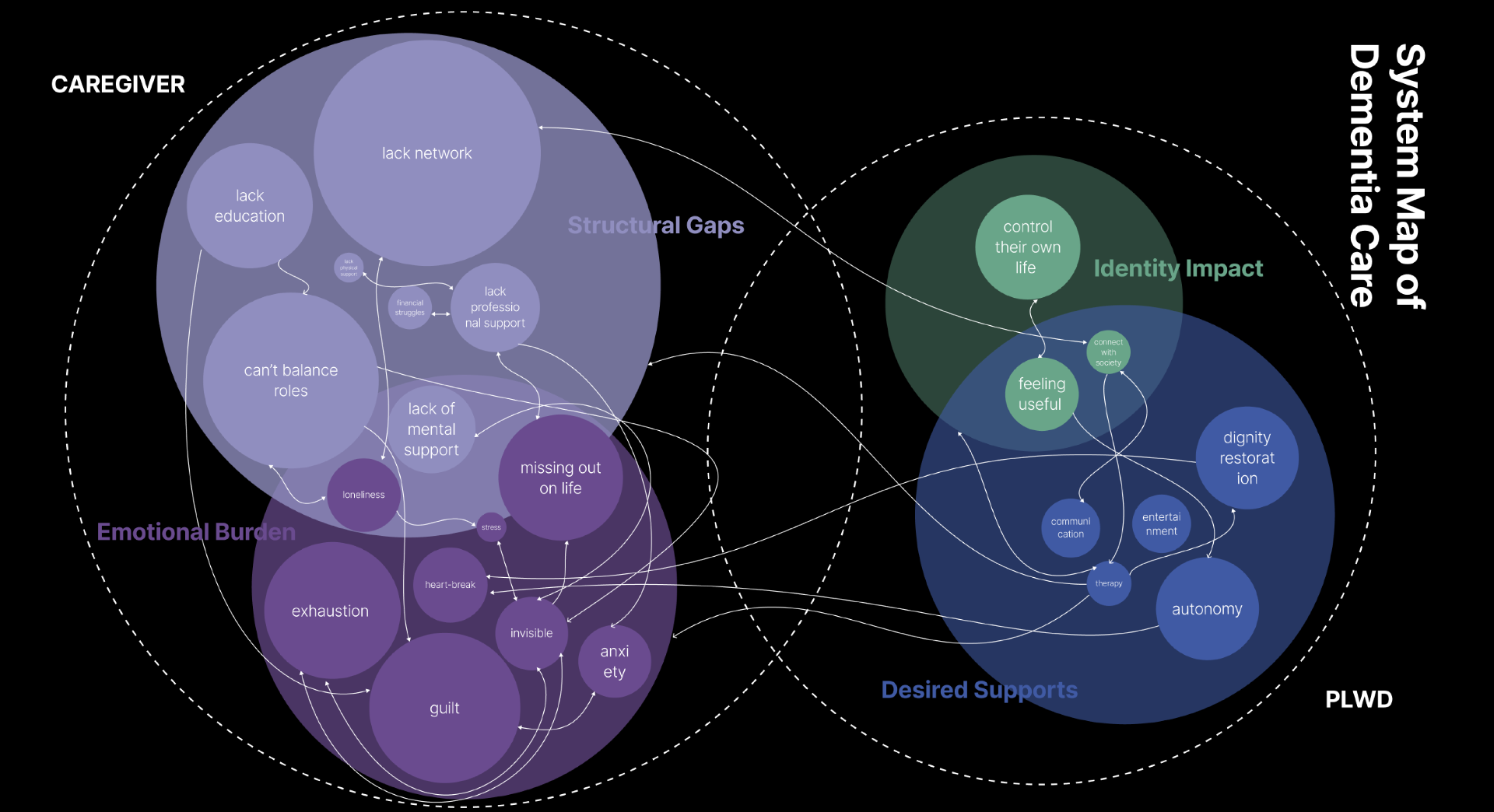
The most repeated emotional patterns were guilt, exhaustion, missing out on life, loneliness, and anxiety. In terms of structural gaps, it became clear that stronger networks, a better ability to balance roles, more support, and better education could make a significant difference. It is also important to recognise that, in some of these areas, cultural context can play a critical role.
It should also be noted that, although this was not the case in the online case studies, most of the interviewees I spoke with were not facing severe economic difficulty, or had access to relatively good governmental support. Many of them identified this as a significant privilege. Even so, they still described feeling unseen and misunderstood, sometimes even within their closest circles.
The emotional weight of care was repeatedly emphasised. One person said:
"It was like I was always in on-call mode."
Another said:
"We couldn't have a proper meal together, relaxed."
At the same time, many of them felt guilty, not enough, or even useless, while also being constantly anxious about hazards or unpleasant events that might happen. One of the main consequences of all these pressures was damage to other relationships in their lives, as well as their own needs becoming less of a priority.
When I asked where these difficulties came from, what might improve them, or how they could be better managed, three main themes kept returning: awareness, education, and connection. It seemed that a large part of the emotional burden could be reduced, or at least improved, through stronger networks. However, this also came with complications. B said:
"I am in hundreds of Facebook caregiver support groups, but honestly sometimes none of them are useful. Not because they are bad, but because this disease has too many stages and thousands of appearances. I need someone to understand me, my exact mum's situation, and truly be there for me."
Three of my interviewees mentioned a similar point: that they did not know enough about dementia when the journey began, and that better educational resources could have made a real difference. One said, "We didn't know much about this. If there were better educational resources to prepare us, we might have faced it better." Another reflected, "Psychological intervention might have been helpful if we had used it sooner. We lost time. That wasn't something we could handle by ourselves. I wish we had taken a psychological path either for our dad or for myself."
The different patterns I identified did not stand alone. Each issue created or intensified another, and many of them also affected the person living with dementia (PLWD). For instance, a stronger support network could reduce the caregiver's loneliness, while also helping the person living with dementia stay more connected to society, which could improve their mood and communication. Similarly, better education could reduce guilt while also helping caregivers balance their roles more effectively, which might indirectly reduce isolation.
Apart from these emotional burdens and structural gaps, another important issue mentioned by many interviewees was not being prepared for what would happen next. Uncertainty is a major part of the experience of dementia. The variety of symptoms and the wide range of stages make it extremely difficult to predict what is coming or to feel ready for it. This is where the role of awareness, education, and preparation becomes particularly clear.
In the second film I made, my intention was to communicate with adults who have not had this experience, or who are new to this situation, so that they might understand it better, in a way, to encounter it before experiencing it in real life. As one of my interviewees said:
"If we had known how long this journey could be, and how difficult it would be, we might have faced it more realistically and more efficiently."
Translating Research into Practice
Each story brought its own unique arc. Because the interviews happened in a free-flowing, storytelling style, they allowed each experience to unfold in its own way. I became familiar not only with the facts of what had happened, but also with the characters involved, the emotional ups and downs, the challenges each caregiver faced, and the ways they tried to respond to them.
I believe the direction of the project was shaped by both the content and the form of the interviews. My initial intention was to use design as a tool to propose something that could help people living with dementia live a better life. However, through the interviews, it became clear that the overlooked experience of caring for a person living with dementia could itself be one of the most important starting points for offering any meaningful support.
A simple idea became central to the project: first we have to see the issue clearly, and only then can we begin to respond to it properly.
This shifted my direction from designing an immediate product or tool towards speaking about this overlooked and unseen anchor of care through artistic practice. The choice of creative writing and filmmaking as methods also came from the style of the interviews themselves. People shared their stories with me, so I responded by working with story, voice, image, and atmosphere.
Rather than only explaining the topic or bringing it to the surface in a direct way, my intention became to create an encounter for adults who have not experienced this situation, as well as for new caregivers. Through fragments of similar stories gathered from different human experiences, cultural backgrounds, and family situations, the work tries to communicate something of what caregiving feels like before someone is fully inside it.
Many interviewees mentioned that not having any real idea of what this situation could become, until they were suddenly placed in it, made the experience harder to manage. This became one of the key reasons for translating the research into film: to make space for awareness, recognition, and emotional preparation before the crisis fully arrives.
Reflection
The most significant finding, and the one that shifted both the direction of the project and my own perception, was this: caregivers also need to be cared for.
Statistics and existing research show that dementia is growing globally every year, which makes it increasingly important to study, discuss, and design for this condition. However, the more I focused on this area, the more I realised that unpaid caregivers, as an essential pillar within the community of care, are still often overlooked. This absence appears not only in systems of support, but also across academic research, product design, and artistic narratives.
Considering the diversity of the people I interviewed, across different countries and backgrounds, it was surprising to see how many similar experiences, feelings, and challenges appeared. This made caregiving feel like a shared human condition. Each story was unique, but many of the emotional patterns were common: exhaustion, guilt, loneliness, uncertainty, responsibility, and the gradual loss of personal space and time.
I also found that caregivers could often understand one another very quickly, even across cultural differences. The community itself was deeply understanding, despite the very difficult situations its members were facing. Many caregivers, especially those with past or longer experience, wanted to help others in similar situations. They shared knowledge, wrote books, ran workshops, joined online groups, used social media, and tried to connect people who might understand each other's emotional load.
I found this community supportive and caring, not only towards the people they were looking after, but also towards other caregivers. I was often asked how I managed to speak with so many people in such a short period of time, around one to two months. For me, this was possible because of the generosity of caregivers themselves. Many were eager to share their experiences, challenges, and journeys because they believed that more knowledge could make the path less lonely and less shocking for someone else.
At the same time, as a short film, my work cannot capture every aspect of each individual situation in detail. It also does not categorise caregiving according to the stage of dementia, the symptoms of the person living with dementia, or the specific circumstances of each family. Therefore, I see the film as a broader narrative representation of caregiving: its emotional weight, burnout, invisible labour, and the difficult moments that many caregivers may recognise, even if their exact situations are different.
An actual solution or support tool that responds to this lack of preparation and ongoing uncertainty is still missing. However, I see this film as the first step in a longer journey. By showing the reality of this condition to audiences who may be unfamiliar with it, the work creates a moment to pause, reflect, and recognise the hidden labour of care.
This is not an end product or a complete solution. It is an outcome from one stage of research, and a small but meaningful intervention within a longer process of asking how the whole community of care might be better supported.
Possible Ways of Supporting Unpaid Caregivers
Through the interviews and shared stories, it became clear that support for unpaid caregivers cannot be reduced to one simple solution. The needs that appeared were emotional, practical, social, financial, physical, relational, and deeply personal. Caregivers were not only asking for more services, but for more recognition, clearer information, moments of rest, and spaces where their own lives could still exist alongside the role of care.
From their perspectives, help can begin with emotional support: feeling seen, being listened to without judgement, and having space to express anger, guilt, grief, exhaustion, and loneliness. Many caregivers described the emotional weight of care as something that is difficult for others to understand unless they have lived it themselves.
Another repeated need was informational support. Many caregivers spoke about not knowing what to expect, especially after diagnosis or during moments of change. Better understanding of dementia, its stages, available services, legal and medical processes, and how to respond in difficult situations could reduce fear, guilt, and uncertainty.
There is also a strong need for practical and institutional support. This includes help with routines, appointments, medication, paperwork, respite care, and easier navigation of services. Several stories showed how caregivers often become responsible not only for emotional care, but also for administration, decision-making, coordination, and constant problem-solving. This labour is often invisible.
The research also points to the importance of social and relational support. Caregivers need connection with others who understand their situation, but they also need help managing changing family dynamics, conflict, guilt, and the difficult shift between love and responsibility. Support groups and online communities can be helpful, but more when they feel specific and relevant to the caregiver's actual situation.
A further area is identity-based support. Many caregivers described feeling as if their own life, interests, time, and future had slowly disappeared into the role. Support, therefore, should not only help them care better, but help them remain connected to themselves beyond care.
Finally, one of the strongest themes was the need for support before things become overwhelming. Many caregivers said they were not ready for the scale, length, and emotional difficulty of the journey. This suggests a need for tools, experiences, or spaces that help people understand what caregiving may involve before they are fully inside it.
These findings open possible directions for the next stage of the project. Rather than searching immediately for one fixed product or solution, the research suggests that any future design intervention should respond to the layered nature of care: emotional, practical, social, temporal, and bodily. The question now becomes how design can create forms of support that help caregivers feel less alone, more informed, more recognised, and more able to continue without disappearing into the role.
Together, these areas show that caregiving support must be designed as a system of care around the caregiver, not only around the person living with dementia.
Moving Forward
Based on my interviews, bringing this topic to the surface and opening it up is already an important step. Several participants reflected that simply seeing or hearing from someone in a similar situation could have changed how they experienced the beginning of their caregiving journey.
As A said:
"If I had seen someone in a similar situation to mine, I might have handled things better. I felt completely naive when I was suddenly put into this situation without expecting it."
N also spoke about the need for a wider cultural shift:
"The culture needs a shift. We have to accept and expect that we, us and our loved ones, are going to live longer, and those last years will not necessarily be easy or quick. We must prepare ourselves for it. If we do that before we face it, maybe we can pass through it more smoothly."
The next step is to add another layer to this possibility and bring more depth to it. If the current stage of the project has focused on visibility, reflection, and emotional recognition, the next phase will ask how this awareness can become a more practical form of support.
The main goal of the project is to support new caregivers by helping them feel more prepared, and more broadly to support caregivers who are facing unwanted stress, uncertainty, and emotional pressure. In the next phase, I will explore how this support could be translated into a practical tool, framework, or experience.
The interviews will remain the concrete foundation of the process. I will continue to build from caregivers' lived experiences, using the concept of creative care to shape a process that is not only about representing care, but also about finding ways to support those who give it.